- March 18, 2026
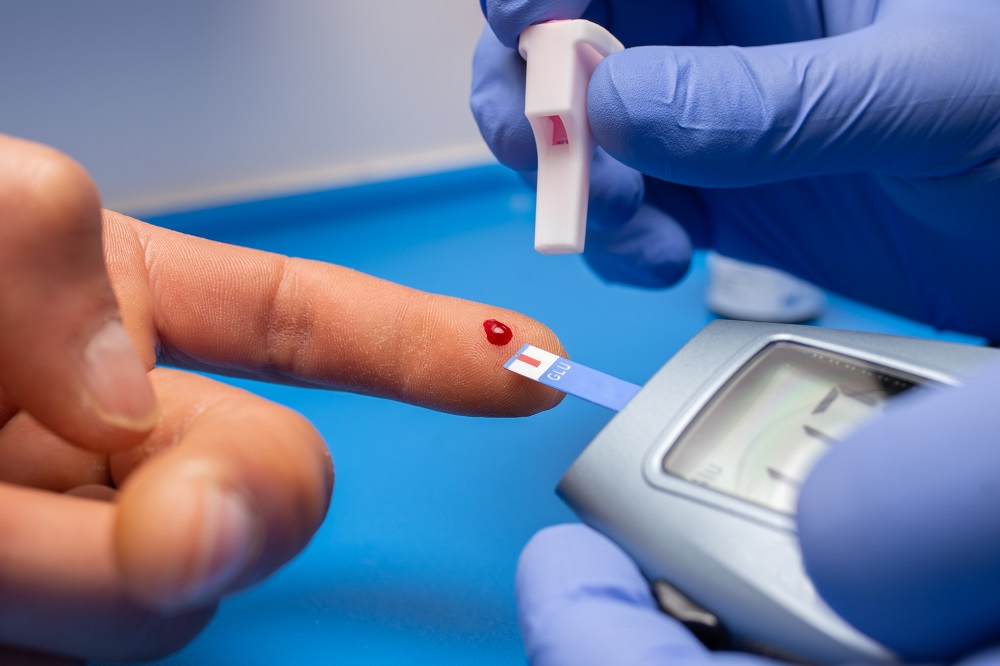
Diabetes is a chronic condition where the body cannot properly regulate blood sugar (glucose) levels. This happens either because the body does not produce enough insulin or cannot use it effectively. Over time, uncontrolled diabetes can lead to serious complications such as heart disease, kidney damage, nerve problems, and vision loss. It is diagnosed through blood tests and managed through lifestyle changes, medications, and regular monitoring under the guidance of a primary care provider.
Diabetes is one of the most prevalent chronic conditions worldwide, and one of the most manageable when addressed early and consistently.
Yet, despite advancements in treatment, diabetes continues to rise at an alarming rate. According to recent global estimates, over 537 million adults are living with diabetes worldwide. This number is expected to reach 643 million by 2030.
What makes diabetes particularly challenging is not just its prevalence, but its long-term impact on multiple organ systems.
This is where primary care plays a critical role, offering continuous monitoring, early intervention, and personalized management.
What is Diabetes?
Diabetes is a chronic metabolic condition characterized by elevated blood glucose (sugar) levels due to problems with insulin production, insulin function, or both.
Diabetes is one of the most common chronic conditions managed in primary care and is a major contributor to long-term health complications when left uncontrolled. Many patients at Windermere Medical Group are diagnosed during routine check-ups, often before symptoms become severe. Early detection is critical, as timely management can significantly reduce the risk of complications.
As a comprehensive family clinic in Georgia offering both primary care and urgent care services, Windermere Medical Group focuses on preventive care, early diagnosis, and ongoing chronic disease management. Our goal is to help patients maintain stable blood sugar levels, improve quality of life, and prevent complications through personalized treatment plans and continuous support.
What Are the Different Types of Diabetes?
Diabetes is not a single condition but a group of metabolic disorders that affect how the body uses glucose. Each type has different causes, risk factors, and management approaches. Understanding the type of diabetes is essential for developing an effective treatment plan.
At Windermere Medical Group, we diagnose and manage all major types of diabetes, ensuring patients receive tailored care based on their condition.
1. Type 1 Diabetes
- Autoimmune condition
- Body does not produce insulin
- Requires lifelong insulin therapy
2. Type 2 Diabetes (Most Common)
- Caused by insulin resistance
- Often linked to lifestyle factors
- Can be managed, and sometimes reversed in early stages
3. Prediabetes
- Blood sugar levels are elevated but not high enough for diagnosis
- A critical stage where intervention can prevent progression
4. Gestational Diabetes
- Occurs during pregnancy
- Increases risk of future Type 2 diabetes
What are the Causes of Diabetes?
Diabetes develops due to a combination of factors rather than a single cause. Understanding these causes helps in both prevention and management.
Lifestyle Factors
Daily habits play a significant role in the development of diabetes, especially Type 2.
- High sugar and processed food intake
- Physical inactivity
- Excess body weight
Genetic Factors
Some individuals have a higher genetic predisposition to diabetes, making them more susceptible even with moderate lifestyle risks.
- Family history
- Ethnic background
Medical Conditions
Certain underlying conditions increase diabetes risk by affecting metabolism and insulin function.
- High blood pressure
- High cholesterol
- Hormonal disorders
What Are the Symptoms of Diabetes?
Diabetes symptoms can develop gradually, especially in Type 2 diabetes, making them easy to overlook. Some patients may not notice symptoms until blood sugar levels are significantly elevated. Recognizing early signs is important for timely diagnosis and treatment.
If you experience any of these symptoms, it’s important to schedule a primary care visit for evaluation.
- Frequent urination
- Increased thirst
- Unexplained weight loss
- Fatigue
- Blurred vision
- Slow-healing wounds
Why Is Diabetes Dangerous?
Diabetes can affect nearly every organ system in the body if left unmanaged. High blood sugar damages blood vessels and nerves over time, leading to serious complications.
Cardiovascular Risks
Diabetes significantly increases the risk of heart-related conditions.
- Heart disease
- Stroke
Kidney Damage
Long-term diabetes can impair kidney function.
- Chronic kidney disease
- Risk of dialysis
Nerve Damage
High blood sugar affects nerve function.
- Tingling or numbness
- Loss of sensation
Eye Complications
Vision can be affected due to damage to small blood vessels.
- Diabetic retinopathy
- Vision loss
Diabetes Diagnoses
Accurate diagnosis is the first step toward effective management. Primary care providers use standardized tests to confirm diabetes and assess severity.
Common Diagnostic Tests
| Test | Purpose |
| Fasting Blood Sugar | Measures baseline glucose |
| HbA1c | Average glucose over 3 months |
| Oral Glucose Tolerance Test | Measures response to sugar |
Additional Evaluations
To assess overall health and risk factors, additional tests may be performed.
- Cholesterol levels
- Kidney function tests
How Is Diabetes Managed in Primary Care?
Diabetes management in primary care goes far beyond simply prescribing medication. It is a comprehensive, long-term care model focused on stabilizing blood sugar levels, preventing complications, and improving overall metabolic health.
Primary care providers act as the central coordinators of care, continuously tracking a patient’s progress, adjusting treatments, and addressing related conditions like hypertension, high cholesterol, and obesity.
1. Lifestyle Management: The Foundation of Diabetes Care
Lifestyle intervention is the most powerful and often the first step in managing diabetes—especially in prediabetes and early Type 2 diabetes.
Rather than short-term changes, the focus is on sustainable, long-term habits that improve insulin sensitivity and metabolic balance.
Nutrition (Medical Nutrition Therapy)
Diet directly impacts blood sugar levels, making it one of the most important components of diabetes care.
- Emphasis on low glycemic index foods
- Increased intake of fiber-rich foods (vegetables, whole grains, legumes)
- Balanced meals with protein, healthy fats, and complex carbohydrates
- Reduced intake of refined sugars and processed foods
Medications
When lifestyle changes are not sufficient, medications are introduced to control blood sugar levels.
- Oral medications
- Insulin therapy
Monitoring
Regular monitoring ensures that treatment remains effective and complications are prevented.
- Blood sugar tracking
- Routine follow-ups
Physical Activity
Regular physical activity improves how the body uses insulin and helps lower blood sugar levels naturally.
- At least 150 minutes of moderate-intensity exercise per week
- Activities like walking, cycling, swimming, or strength training
Weight Management
Excess body fat, especially around the abdomen, is strongly linked to insulin resistance.
- Even a 5-10% weight loss can significantly improve blood sugar levels
- Helps reduce the need for medications in some patients
Sleep & Stress Regulation
- Poor sleep increases insulin resistance
- Chronic stress raises cortisol, which elevates blood sugar
Ways to Control Blood Sugar Naturally
While medical treatment is important, many patients can significantly improve their condition through consistent lifestyle habits. Natural strategies focus on stabilizing blood sugar and improving overall metabolic health.
Dietary Habits
A balanced diet helps prevent spikes and crashes in blood sugar levels.
- Prioritize whole, unprocessed foods
- Include protein and fiber in every meal
- Limit sugary beverages and refined carbohydrates
- Practice portion control
Physical Activity
Exercise not only lowers blood sugar but also improves insulin sensitivity.
- Walking after meals helps reduce post-meal glucose spikes
- Strength training improves muscle glucose uptake
Everyday Habits
Small, consistent habits can lead to meaningful improvements over time.
- Maintain a healthy weight
- Stay hydrated
- Quit smoking
- Limit alcohol intake
When to Visit a Doctor for Diabetes?
Many individuals delay seeking care until symptoms worsen, but early medical evaluation can prevent serious complications.
Primary care visits are essential not only for diagnosis but also for ongoing management and prevention.
You Should Schedule a Visit If You:
- Experience symptoms like fatigue, thirst, or frequent urination
- Have a family history of diabetes
- Are overweight or physically inactive
- Have high blood pressure or cholesterol
- Are over age 40 and have not had a recent screening
Personalized Diabetes Management for Long-term Health
Managing diabetes effectively requires a healthcare provider who offers continuity, accessibility, and personalized care. Windermere Medical Group provides a comprehensive approach tailored to each patient’s needs.
What Sets Our Care Apart
- Integrated primary care and urgent care services
- Personalized, long-term treatment plans
- Preventive screenings and early diagnosis
- On-site lab testing for convenience
- Accessible care across Georgia
Trusted Medical Care, Wherever You Are
With established offices in:

Conclusion
Diabetes management is a continuous process that requires awareness, consistency, and the right support system. With the guidance of a primary care provider, patients can effectively manage their condition and reduce the risk of complications.
The combination of:
- Healthy lifestyle choices
- Appropriate medications
- Regular monitoring
FAQs:
Q1. What is the best way to manage diabetes in primary care?
The best approach includes lifestyle changes, regular monitoring, medications if needed, and continuous follow-ups with a primary care provider for long-term control.
Q2. Can Type 2 diabetes be reversed with primary care treatment?
Early Type 2 diabetes can often be improved or reversed with weight loss, a healthy diet, and physical activity under consistent primary care supervision.
Q3. How often should I visit a doctor for diabetes management?
Most patients should visit every 3-6 months, depending on blood sugar control, treatment plan, and presence of complications.
Q4. What foods help control blood sugar levels?
Foods high in fiber, lean protein, healthy fats, and low glycemic index carbohydrates help maintain stable blood sugar levels.
About the Author

Priya Bayyapureddy
Dr. Priya Bayyapureddy, MD is a board certified Internal Medicine doctor with over 20 years of experience in primary care Internal Medicine. Dr. Bayyapureddy completed her Internal Medicine residency at Emory University School of Medicine and internship at University of Tennessee College of Medicine at Chattanooga.
Recent Post





